Céphalées
De médecine.top
Céphalées primaires
Migraine
Test rapide de la migraine
- Lors des trois derniers mois, est-ce que vos activités ont été limitées un jour ou plus suite à une migraine ?
- Pendants vos céphalées, souffrez-vous de nausées ou vomissements ?
- Est-ce que la lumière vous dérange lorsque vous souffrez d'une migraine ?
Si 2/3 questions répondues par oui → 93% de probabilité que la personne souffre de migraines[1]
Caractéristiques
- Unilatérale, pulsatile
- (Assez) sévère
- Symptômes végétatifs ++
- Anorexie, vomissements
- Photo/phonophobie
- Augmentation des douleurs avec mouvements de la tête
- Patient veut se retirer dans l’isolement
- Formes épisodiques vs chronique
- 20% avec «aura»: symptômes neurologiques focaux progressifs sur 5-20 min.[2]
Prophylaxie
- Metoprolol, propranolol, timolol, divalproex sodium, and topiramate all have Level A evidence for prevention of episodic migraine and should be considered for migraine occurring at a frequency of at least 5 days per month.[3]
Traitement de la crise aiguë
- AINS
- For patients with a history of episodic migraine with typical aura that no longer responds to appropriate NSAIDs, guidelines recommend the use of triptans.
- Par exemple: Imigran® spray nasal 1×10/20 mg dans une narine, répéter après 2h, max 40 mg/24h
Traitement au long cours
Céphalées de tension
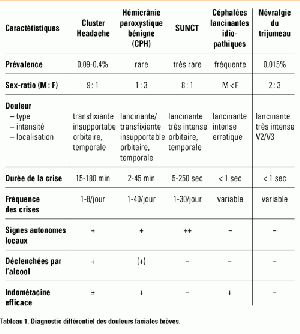
Céphalées trigéminales autonomes
Cluster headache
- Cluster headache, the most common of the trigeminal autonomic cephalalgias, is best prevented with verapamil.
Hémicrânie paroxystique bénigne
SUNCT
Céphalées lancinantes idiopathiques
Synonymes: primary stabbing headache, "ice-pick" headache
- Indomethacin may be helpful during cycles of repeated occurrences but is rarely necessary.
Céphalées secondaires
Red flags
- First or worst headache
- Abrupt-onset or thunderclap attack
- Progression or fundamental change in headache pattern
- Abnormal physical examination findings
- Neurologic symptoms lasting longer than 1 hour
- New headache in persons younger than 5 years or older than 50 years
- New headache in patients with malignancy, coagulopathy, immunosuppression, or pregnancy
- Association with alteration in or loss of consciousness
- Headache triggered by exertion, sexual activity, or Valsalva maneuver
Céphalées en coup de tonnerre
Hémorragie sous-arachnoïdienne
Thrombose d'un sinus intra-crânien
- Treatment with low-molecular-weight heparin results in lower hospital mortality than treatment with unfractionated heparin. Anticoagulation with warfarin is generally continued for a minimum of 3 to 6 months. Extended anticoagulation should be considered in those with severe hypercoagulable states, myeloproliferative disorders, or recurrence and perhaps in those with idiopathic thrombosis.
Névralgie du trijumeau
- Carbamazepine is the treatment of choice for trigeminal neuralgia; management with this agent requires serum monitoring for hyponatremia and agranulocytosis.
Références
- ↑ Prof Annoni, HFR
- ↑ Cours médecine Prof Philippe Ryvlin et Patrik Michel, UNIL CHUV
- ↑ https://mksap18.acponline.org/app/topics/nr/mk18_a_nr_s1/mk18_a_nr_s1_4